Chinese Wild Yam: A Nourishing Root

There are many yam varieties throughout the world that hold various therapeutic benefits which range from boosting the immune system to supporting fertility.
There are many yam varieties throughout the world that hold various therapeutic benefits which range from boosting the immune system to supporting fertility. One in particular, the Chinese wild yam root, dioscorea radix, or shan yao in pinyin has a few notable medicinal properties which make it popular to use in Chinese herbal formulas. As a root and a relatively sweet and sticky one at that, Chinese medical theory recognizes shan yao as being useful for nurturing the ‘root’ of our bodily organs, also known as the kidneys.
Shan yao has the benefit of ‘restraining the essence.’ This points to its aspect of supporting the root, or kidneys. The kidneys act as a foundation to our body’s complete vitality. When the kidneys are solid and strong, all other organs have a greater capacity to flourish in health. Yam also nourishes the lungs and spleen especially in cases of loss of fluids as in excessive urination, abnormal discharge, abnormal sweating, diarrhea, and weak digestion.
Taken as a porridge, shan yao is beneficial for ‘wasting and thirsting disorder’, also known as diabetes. A study published in the Archives of Pharmacological Research noted that Chinese wild yam has the capability of improving digestion by promoting the proliferation of beneficial gut bacteria in cases of hyperlipidemia and hyperglycemia. (Jeon, et al., 2006)
Coldness and dryness permeate the winter season, bringing with it the conditions such as dry cough, excessive thirst, and often fatigue. Adding to its moistening benefits, Chinese wild yam is an excellent herb for supporting the lung qi and lung yin, such as in cases of asthma or dry chronic cough.
It is only fitting that yam is so valued as a nourishing tonic within many dishes including soups and stews in the cold months during the fall and winter. One very simple way to add yam to the diet is this basic baking method of preparing the yam:
Preheat oven to 400
Cube 2 yams and cover with 2 tablespoons ofdesired fat (butter, ghee, non-gmo canola oil, coconut oil)
sprinkle 1/2 tsp salt, 1/2 tsp pepper, 1/2 tsp garlic powder
Bake until cubes are softened, about 30 minutes
1. Belanger, Charles. The Chinese Herb Selection Guide. Phytotech, Richmond, Ca. 1997. pp. 796-797.
2. Jeon JR1, Lee JS, Lee CH, Kim JY, Kim SD, Nam DH. Effect of ethanol extract of dried Chinese yam (Dioscorea batatas) flour containing dioscin on gastrointestinal function in rat model. Archives of Pharmacal Research. 2006 May;29(5):348-53.
Colorectal Cancer: Do You Know The Facts?
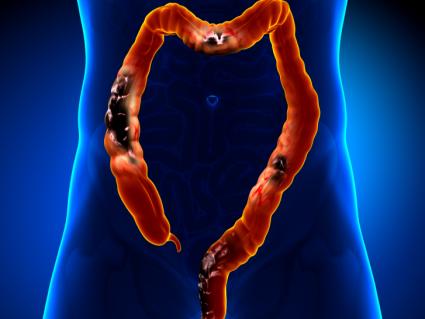
Colorectal cancer is the third most common cancer in the United States.
March is colorectal cancer (CRC) awareness month! Did you know that colorectal cancer is the third most common cancer in the United States? Men and women have an equal risk for developing the disease—a risk of about 1 in 20.
Although some risk factors for CRC cannot be changed, such as age older than 50 years, African American race, personal and family history of CRC or polyps, and inherited syndromes (familial polyposis and Lynch syndrome), lifestyle risk factors, including nutrition, can be modified. Lifestyle risk factors for CRC include eating a low-fiber, high fat diet (Standard American Diet), sedentary lifestyle, obesity, and tobacco and alcohol use. The metabolic syndrome, specifically hyperinsulinemia, has been linked with a higher chance of CRC. A study in the Archives of Internal Medicine showed that those who eat the typical Standard American Diet featuring red meat, sweets, desserts, fried foods, and refined grains had a 50% greater chance of developing CRC than those who consumed few of those foods.
We know that up to 70% of CRC cases can be prevented by the following diet and lifestyle changes: avoidance of red meats (especially charred), processed meat, and refined carbohydrates; maintenance of healthy body weight (body mass index less than obese); avoidance of hyperinsulinemia/metabolic syndrome; maintenance of recommended activity levels; and avoidance of alcohol and tobacco. Nutrition should focus on a whole-food plant-based diet, such as the Mediterranean or Anti-inflammatory diet. A diet high in fiber, fruits and vegetables, and fish, and low in red meats is protective against CRC.
In patients who have had early stage CRC and underwent standard therapy, prospective observational studies have shown that increased exercise after diagnosis, avoidance of a Standard American Diet, lower glycemic load diet, eating calcium-rich foods, and increased vitamin D levels were associated with a reduced risk of cancer recurrence and improved overall survival.
Several nutrients have demonstrated protective effects for CRC; some of these include garlic, curcumin, flaxseed meal, folic acid, indole-3-carbinol (in cruciferous vegetables), L-glutamine, mushroom extracts (maitake, reishi, Cordyceps, and others), omega-3 fatty acids (EPA and DHA), probiotics, quercetin, resveratrol, as well as vitamin D and calcium.
Taking a proactive nutritional approach by eating a plant-based, whole-foods diet rich in fiber and low in glycemic index is a prudent part of decreasing CRC risk for us all.
Community Acupuncture Relieves Stress
Community Acupuncture has been a powerful ally in helping our community to unwind. Stress is one of the most common symptoms of this day and age. Its side effects can include such symptoms as: depression; headaches; acid reflux; anxiety; poor memory and trouble sleeping. Stress can subtly creep into our lives or may be directly related to specific events or thought patterns.
Conveniently, the Center is offering Community Acupuncture, which is proving to be very popular in the area because of it reduced cost. At the Center, walk-ins are welcome if we can accomodate but appointments are encouraged. This is perfect if you are having a challenging day and need relief. Acupuncture is an excellent way to effectively release stress, and provides an individual a natural, drug-free way to relax almost instantly.
Community Acupuncture Update
Community acupuncture is off to a great start at the Center. We still have room for new patients, but the initial response has been even greater than expected. Clients are coming in to experience group acupuncture, in some cases bringing along a daughter, brother, mother or friend to explore it with, and leaving very relaxed and happy.
This is a new program for the Center, and we weren’t entirely sure how all the logistics would play out, but everything has gone exceptionally smoothly. The room has come together very nicely thanks in large part to Nadine and Rebecca’s aesthetic sensibilities, and already has the charged feel of a healing space.
It is a deeply satisfying joy to move through a room of clients immersed in an experience that began thousands of years ago. The connection to the past and to each other is all but palpable in the room. I would like to thank all who have come to join us thus far to make this possible, and look forward to all the new faces we’ll be seeing in the future.
Confronting Ageism

As an individual naturally progresses through life, resilience is tested as acts of discrimination and prejudice against a person on the bases of age increases. Much research has concluded that negative stereotypes about older people are a direct threat to cognitive abilities in later life. Through the world of separating people into groups of high and low risk solely on the bases of age, there is further divide. Promoting healthy aging for older adults during the world of COVID-19 can include minimal contact with loved ones, and the overwhelming sense of anxiety that your life path could abruptly end without the proper goodbyes to those you love. We are aging in a new world now, and it is important to be mindful of the challenges you could experience...
In a study presented by Hess, Hinson, and Statham (2004), young and old individuals were exposed to explicit and implicit age-related stereotypes and then tested on their memory recall skills. The results concluded that when older participants’ witness age-related stereotypes, there is significant decrease in memory recall compared to younger participants. This then brings us to the question—how do we expect older people to retain their optimism when they are constantly bombarded with prejudice regarding their cognitive, physical, and emotional abilities? Ageism infuses itself into all areas of society; therefore, infuses itself into the unconscious mind of the aging individual.
The last year and a half have taught us how unbelievably precious life can be. Potentially the most critical lesson we have learned is how important social interaction is for a positive and happy life. One of the many devasting consequences of COVID-19 is the impact on the mental health of our older population. COVID-19 has been shown to lead to memory impairment, loss of alertness, increased anxiety, and decline in physical function among the older population. The loss of stimulation for those in this population instantaneously decreased psychosocial wellbeing, leading to an influx of decline among our already vulnerable population.
Psychological stress induced by COVID-19 needs to be understood at all levels of health care. We need to pay more attention to our older adult population and guide them through the obstacles that they may experience. When we recognize that there are parts of our society that negatively impacts one group of people more than another, then true change can occur. Research shows that improvements in the physical and mental health of older people can occur when we educate all ages of society about the myths associated with aging.
We need to emphasize that all life is beautiful—all life is worthy of love, admiration, and appreciation regardless of age, sex, gender, race, and ethnicity. As time moves on, healthy aging is our navigation. A healthy aging is embracing the grace of age with all of its trials and tribulations.
Sources
1. Nelson, T.D. Promoting healthy aging by confronting ageism (2016). American Psychological Association, 7(4): 276-282.
2. Batsis, J. A et al. Promoting healthy aging during COVID-19. (2021). Journal of American Geriatric Society, 69(3): 572-580.
Confronting Ageism Related Blog Posts
Confronting Ageism Related Services

Anti-Aging Therapy
How to Combat the Anti-Aging Process with Intravenous (IV) Therapies As we get older how do we combat the natural effects of the aging process?First, we have to look at some of the main factors that cause the symptoms of aging and degeneration. These symptoms include fatigue, muscle weakness or muscle loss, reduced stamina and endurance, poor memory and cognition, and chronic inflammation and…Anti-Aging Therapy

Mental Health Counseling
At the Stram Center, we recognize that mental health is often the basis of your potential to navigate life’s challenges as well as to heal from physical illness. Understanding your full self, including traumas and difficulties you may have experienced, is often the first step to learn what your unique strategies are in the face of life’s difficulties. Quality healthcare should include support…Mental Health Counseling
Connecting Through Gratitude & Grace

The power of gratitude.
The Chinese character for gratitude includes a pictogram of the heart 心 indicating that this is a notion that connects to our center of emotional intelligence. To give thanks freely is to acknowledge the depth of feeling of gratitude stemming from the heart.
I think of showing gratitude as a way to connect someone or something else to the grace in your own heart. Expressing gratitude has a calming affect on oneself and the recipient of the gratitude. Also, there is evidence that this creates positive physiological responses in our body. A 2017 study published in Scientific Reports attributes living a life of gratitude to a lower incidence of psychiatric issues, higher satisfaction in life, and wisdom. The research team was able to analyze the physical impact of gratitude versus resentment through MRI and pulse analysis. They found that the act of gratitude reduces heart rate and increases neural connectivity, compared to acts of resentment which have the opposite affect. In other words gratitude increases happiness and self awareness. Furthermore, these feelings are catching. When we deliver gratitude, those around us can be inspired to do the same.
Reference:
Kyeong, S., Kim, J., Kim, D. J., Kim, H. E., & Kim, J. J. (2017). Effects of gratitude meditation on neural network functional connectivity and brain-heart coupling.Scientific reports,7(1), 5058. doi:10.1038/s41598-017-05520-9心
Connecting With Our Connective Tissue

Listening to and caring for our connective tissue.
Taking time for your emotional and physical health is a great way to start the new year. It is important for all of us to take time to rejuvenate, recharge and listen to our tissues.
Our bodies communicate daily through signals. Sitting for long periods of time, rounding your shoulders while working, feeling stressed and clenching your teeth are actions which send signals that may create symptoms like headaches, sore shoulders, back pain, neck and jaw pain. These symptoms are restrictions in your connective tissue which can lead to asymmetries in the body causing excess pressure on nerves, muscles, vessels and organs. This pressure leads to the signal that is pain.
The connective tissue in your body is a water-based, body-glide system. The tissue needs fluid to move. If you are feeling achy, try drinking water. Staying hydrated can relieve headaches and body pains.
A massage is a great way to reconnect with your body. Massage releases holding and bracing patterns, reduces pain and increases mobility to help restore balance to your body so it can function optimally. Massage can also help boost immunity, reduce anxiety or depression, stimulate the lymphatic system and increase circulation.
Listen to your body’s signals and feel your best in 2020.
Cooling Off at the Pool: Large Intestine 11
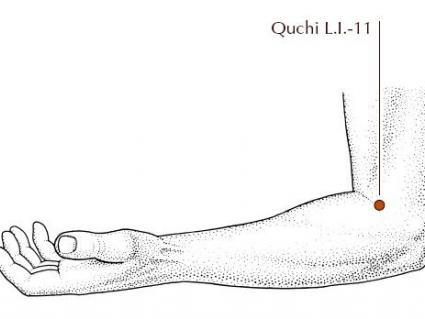
Did you know you have a "pool" in your arm that can help you keep cool in the summer?
As summer heat comes near, we are reminded of the blissfully refreshing havens that are our favorite lakes, ponds, pools, or oceans. Acupuncture has some pools of its' own, one of which is known as Qu chi, or "Pool at the Bend." Located along the large intestine channel, it is one of the most commonly used points to cool and clear heat from the body. Whether it is heat and irritation from a poison ivy rash, a headache from staying out too long in the sun, or simply too much spicy BBQ leading to heartburn, this "pool at the bend," is called upon to help the body clear excessive heat in many ways.
The point is found where the crease of our elbow joint ends when flexing the arm to lift a cold beverage to our lips (or curl a dumbbell). Rather than applying pressure to the point, use a clean fingernail or even a soup spoon (called gua sha in traditional acupuncture) to scrape the point gently. You just need to scrape until the skin reddens slightly - do not break or damage the skin. The "small heat" of the scraped skin draws out the "big heat" within the body so that it can be cleared out. And of course, hydration, shade, and rest when needed will keep summer fun!
Covid Prevention: How to Keep Yourself Safe During the Second Wave

The holiday season is upon us, but unfortunately, the rate for Covid infections, hospitalizations, and fatalities are at an all-time high. The U.S. is adding close to 300,000 new cases per day and close to 3,000 fatalities per day1. Until we can get vaccinated, we still need to take measures to prevent infection. A protocol based guide for recommended treatment and prevention of COVID was recently written by the Chief of Pulmonary and Critical Care Medicine at Eastern Virginia Medical School (EVMS). In the guide, many of the recommendations for prevention are natural therapies. I will discuss two of the therapies recommended in this post, vitamin D and melatonin. By combining natural therapies with mask wearing and social distancing, we can help reduce the spread of infection. We know that vitamin D is an important vitamin for bone health. But vitamin D also plays a critical role in immune function
An article published in September of 2020 found that blood levels of vitamin D of at least 30ng/mL (normal range is 30-100) reduced risk for poor clinical outcomes2. Pneumocytes are specialized cells in the lungs that produce surfactant which protects against acute respiratory distress syndrome. COVID virus targets these cells leading to decreased surfactant levels. Vitamin D reportedly helps to reduce destruction of pneumocytes and stimulate surfactant production which can prevent severe lung injuries3. Vitamin D can also play a role in reducing inflammation. It can reduce inflammatory markers such as c-reactive protein (crp) and reduce inflammatory cytokines such as IL-2, 6, and 12 (interleukins), tnf-alpha, and nf-kappaB. Over production of these cytokines, also known as the “cytokine storm”, is responsible for the symptoms associated with COVID (and the influenza virus). Vitamin D suppresses the release of these cytokines. Vitamin D can also stimulate the production of antimicrobial peptides and specialized lymphocytes that target viruses.
Melatonin is produced in the pineal gland and assists in initiating the sleep cycle. For many years research has shown its effectiveness for fighting cancer due to having anti-inflammatory properties. So how can it help for COVID? It has been found that melatonin is actually produced by mitochondria as well.When cells are undergoing inflammation, they stop making energy through mitochondria and start producing energy primarily from glucose. This leads to a production of more inflammatory cytokines and inhibits production of melatonin. Since melatonin exerts an anti-inflammatory effect, the combination of increased cytokines and decreased melatonin lead to even more inflammation4. When taken as a supplement melatonin can start to reverse this inflammatory cascade. Melatonin production is also decreased in people of older age and therefore may be more susceptible to inflammation and adverse effects of COVID.
Other preventive nutrients mentioned in the EVMS protocol were vitamin C, zinc, and quercetin. These nutrients are well known antioxidants and immune stimulants. At the Stram Center we can do a full evaluation of these nutrient levels and provide the correct guidance for dosing and safety.
1. CURRENT RATES
https://www.nytimes.com/interactive/2020/us/coronavirus-us-cases.html
2.VITAMIN D
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7518605/pdf/pone.0239799.pdf
3.VITAMIN D IMMUNE FUNCTION
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7447609/pdf/12967_2020_Article_2488.pdf
4.MELATONIN
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7211589/pdf/main.pdf
Covid Prevention: How to Keep Yourself Safe During the Second Wave Related Blog Posts
COVID-19 Long haulers Syndrome: Treatment, Symptoms and the Relation to Chronic Lyme Disease.

Researchers estimate about 10% of COVID-19 patients become long haulers (long COVID), according to a recent article from The Journal of the American Medical Association, and research presented by scientists based in the United Kingdom. Whether you are older or younger, healthy or battling other health conditions, or if you had mild or severe COVID-19 symptoms, these conditions could affect anyone. The term “long hauler” is broadly used to characterize individuals whose symptoms persist or develop outside the initial viral infection; the duration and pathogenesis are still unknown, however there are theories. King’s College researchers reviewed their data from the COVID Symptom Study and identified patterns that suggested long-term COVID symptoms were twice as common in women than in men and the median age was 45.
Common Symptoms
Early clinical studies have shown that COVID patients may experience complications like myocarditis(inflammation of the heart), abnormal heart rhythms and other cardiac sequelae weeks after contracting the virus. These conditions may help explain why some long haulers experience shortness of breath, chest pain or their heart racing. Out of all the facets of the corona virus, this one may prove the most difficult to recognize. Long-haul COVID patients carry their symptoms well beyond what we’ve come to understand as a “normal” course of recovery. For some, long-term COVID symptoms can last for weeks, and for others, it has been months—and counting. The persistent symptoms are wide-ranging: they include “brain fog,” memory, attention problems, shortness of breath, racing heart, nausea, diarrhea, intermittent spiking fevers, fatigue, persistent cough, muscle aches, and finally, insomnia. In the journal of Clinical Microbiology and Infection, a two-month follow-up of 150 adults with only mild to moderate COVID cases found that TWO-THIRDS of them were still experiencing symptoms, the most common were shortness of breath, loss of smell and taste, and/or fatigue. If you are experiencing long-term symptoms, call the Stram Center for more information on our treatment for post-COVID patients 518-689-2244 option 2.
Why do COVID-19 Symptoms Persist? Is there a similarity with Persistent Lyme disease?
One common theory about patients with long-term COVID-19 symptoms is that the virus possibly remains in their bodies in some small form. Maybe the simplest explanation for why some long-haulers aren’t recovering is that, even if they test negative, they may in fact still harbor a COVID infection somewhere in their body. Amy Proal, a microbiologist with the PolyBio Research Foundation, focuses on chronic inflammatory diseases, and believes that if people feel sick after an infection, it may be because they in fact are still fighting a hidden infection. “An incredibly logical explanation is that the driving factor is still there,” she says.
A similar argument over what drives chronic symptoms — persistent infection versus lingering inflammation from a past infection — appears prominently in the study of Lyme disease. Some people infected with Borrelia burgdorferi, the tick-borne bacterium that causes Lyme, fail to recover after typical antibiotic treatment. Patients may refer to this illness as “chronic Lyme disease,” and some doctors prefer to call it “post-treatment Lyme disease syndrome,” because they’re not sure an infection is still there. However, in my experience it is in fact that the Lyme bacterium has not been sufficiently irradicated. Unlike typical bacteria, Borrelia Burdorferi is a slow growing bacterium that requires a longer duration of treatment. The controversy stems from the question of the cause of this post-Lyme illness; this very question has resulted in the medical field being polarized for years debating whether treatment was complete, and the post treatment effects are result of the damage from the bacteria and or its inflammatory cascade, versus inadequate, incomplete treatment.
Another theory is their immune systems continue to overreact even though the infection has passed. Unfortunately neither post-Lyme syndrome or Long Hauler Covid-19 have biological markers that allows for concrete diagnosis. The three non-mutually exclusive ideas about what causes long-term symptoms roughly correspond with: a persistent infection (or perhaps merely debris from the Lyme spirochetes or Covid 19 virus ); an autoimmune or inflammatory dysfunction triggered by the infection that continues after virus and bacteria are gone; or changes in the nervous system cells resulting in central nervous system sensitization, where the infection changes how the brain and nervous system respond resulting in once bearable stimuli like touch , light and sound now becoming painful or even unbearable.
Another theory is their immune systems continue to react, even though the infection has passed. The continued reaction may be due to an immune-inflammatory response; the causes are almost certainly multifactorial, but may involve overzealous immune responses, cardiopulmonary or systemic inflammation, vascular inflammation or clotting disorders, and direct damage from viral and bacterial replication during acute illness.
Cytokines play an important role in immune response; however, if too many are released in the blood, they can be harmful, creating the cytokine storm. Again, similar to persistent Lyme Disease, the COVID-19 long-hauler symptoms lead to inflammation and severe illness. Assuming these cytokines, largely produced by monocytes and macrophages, are responsible for enhancing all of this damage, interventions that block their inflammatory activity might prevent long-term COVID symptoms.
For example, an anti-NMDA (NMDA= N-methyl-D-aspartate receptor hypofunction within the brain is associated with memory and learning impairments and psychosis.) receptor encephalitis, the immune system attacks memory and learning neurons in the brain, triggering behavior that resembles what is seen in schizophrenia. It too can be provoked by bacterial and or viral infections. Therefore, treating with prolonged judicious antibiotics and or antiviral therapy may be curative. Moreover, there is also a pediatric condition that is similar to obsessive-compulsive disorder called pediatric acute-onset neuropsychiatric syndrome, or PANS, that many thinks can be set off by infections such as streptococcus, Lyme or another tick borne infection called Bartonella.
One of the drugs used in our practice to reduce the overzealous effects of the immune system like thyroiditis, ulcerative colitis is Low Dose Naltrexone. This drug blocks opioid receptors and is sometimes used to treat autoimmune disease — as well as minocycline used in Lyme treatment, an old antibiotic that also exert an anti-inflammatory, antimicrobial effect in the brain
How Do We Treat COVID Long Haulers Syndrome?
The treatment would also utilize an anti-inflammatory and anti-fibrotic approach to treatment…
Supplemental Therapy: Plays a critical role in immune function.
Vitamin D Supplementation reportedly helps to reduce destruction of pneumocytes and stimulate surfactant production which can prevent severe lung injuries. Pneumocytes are specialized cells in the lungs that produce surfactant a soapy chemical which protects against acute respiratory distress syndrome. COVID virus targets these cells leading to decreased surfactant levels.
Zinc supplementation reduces inflammatory response as well as damage to host tissue. Zinc is involved in the modulation of the master regulator of proinflammatory responses.
NAD+ supplementation plays a key role in regulating the immune responses and functions. Recent studies delineate impaired host NAD+ metabolism during chronic infections and inflammation, suggesting NAD+ replenishment as an avenue to ameliorate deleterious inflammatory responses. Nicotinamide adenine dinucleotide (NAD+) and its reduced form (NADH) play a central role in maintaining cellular metabolism and cell survival.
Vitamin C (ascorbate) is necessary for life. Supplementation improves healing and reduces fibrosis.
Quercetin is the most abundant dietary flavonoid; it has been linked to improved exercise performance and reduced inflammation, blood pressure, and blood sugar levels. Plus, it may have brain-protective, anti-allergy, and anticancer properties. It is reported to be effective on treatment and prophylaxis of other SARS like coronavirus infections, as a strong antioxidant and scavenger flavonoid without any adverse events. Upon this data, the investigators hypothesize that quercetin can be effective on both prophylaxis and treatment of COVID-19 cases.
There is evidence that vitamin C and quercetin co-administration exerts a synergistic antiviral action due to overlapping antiviral and immunomodulatory properties and the capacity of ascorbate to recycle quercetin, increasing its efficacy. Quercetin was also identified as a compound able to block SARS-Coronavirus entry into cells the beneficial effects of quercetin in preventing lung respiratory viral infection
For more information on the COVID-19 prevention pack of supplements, email us: supplements@stramcenter.com Or call 518-689-2244 option 4
Hyperbaric Oxygen Therapy Treatment
Hyperbaric oxygen therapy involves breathing pure oxygen in a pressurized environment.
In a hyperbaric oxygen therapy chamber, the air pressure is increased two to three times higher than normal air pressure. Under these conditions, your lungs can gather much more oxygen than would be possible breathing pure oxygen at normal air pressure.
When your blood carries this extra oxygen throughout your body, this helps fight bacteria and stimulate the release of substances called growth factors and stem cells, which promote healing.
Hyperbaric Oxygen Therapy for Post-COVID-19 Syndrome
Post COVID Brain Fog & Cognitive impairment may be the effect Micro-infarcts and neuroinflammation. These are important causes of local hypoxia (low oxygen), and specifically neurological hypoxia.
One of the options to reverse hypoxia, reduce neuroinflammation and induce neuroplasticity is hyperbaric oxygen therapy (HBOT). We have seen results from HBOT use for those who have brain fog. We have seen patients have full recoveries from consistent hyperbaric use.
Even though many of the beneficial effects of HBOT can be explained by improvement of tissue oxygenation, it is now understood that the combined action of hyperoxia and hyperbaric pressure, triggers both oxygen and pressure sensitive genes, resulting in inducing regenerative processes including stem cells proliferation and mobilization with anti-apoptotic and anti-inflammatory factors.
For more information call 518-689-2244 option 2 to speak with a patient navigator on the benefits of hyperbaric oxygen therapy and brain related issues.
COVID-19 Long haulers Syndrome: Treatment, Symptoms and the Relation to Chronic Lyme Disease. Related Blog Posts
COVID-19 Long haulers Syndrome: Treatment, Symptoms and the Relation to Chronic Lyme Disease. Related Services

Hyperbaric Oxygen Therapy
Dedicated to treating the root cause of illness and using the most advanced integrative methods in a safe environment, the Stram Center for Integrative Medicine, under the medical supervision of Dr. Ron Stram, will utilize the benefits of hyperbaric oxygen therapy (HBOT) to complement and enhance the healing process in both chronic and acute conditions of our patients. You will…Hyperbaric Oxygen Therapy
Integrative Medicine
Integrative medicine is the blending of conventional medicine with holistic, complementary, and alternative medicine. Integrative Medicine is defined as healing-oriented medicine that takes account of the whole person (body, mind, heart and spirit), including all aspects of lifestyle. It emphasizes the therapeutic relationship and makes use of all appropriate therapies, both conventional and…Integrative Medicine

Chronic Illness
Nowhere is the need for an integrative approach more apparent than in the management of chronic illness. We are a synthesis of many systems all working together, and when one or more systems become diseased, all of the others will be stressed as well. From physical challenges, to the challenges of everyday living, to a satisfying quality of life, we have to go past seeing that illness in…Chronic Illness

IV Therapy for Chronic Illness
Chronic illnesses are on the rise in the US. From chronic Lyme disease, cancers, chronic fatigue, pain and more – patients are attempting to live their best lives while fighting a battle within. A patient’s response to chronic illness is unique – based upon many factors ranging from emotional response to the disease, individual physical symptoms, immune response and the duration of the…IV Therapy for Chronic Illness