Lyme Disease

Lyme Disease Diagnosis and Treatment in Delmar NY and Burlington VT offices
At the Stram Center we vow to continue our education on Lyme Disease research, stay up to date on the most effective testing and all the safe available therapies. Moreover, our years of experience in treating patients according to the whole person-integrative medicine approach allows us the most effective way to care for our patients. To see our treatment approach scroll to the bottom!
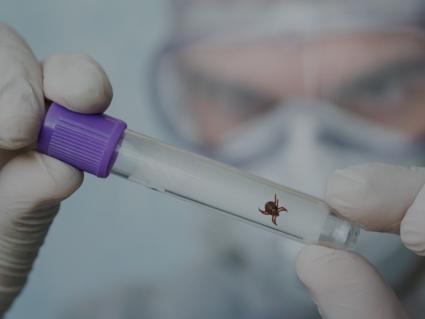
Test Your Tick at TICK REPORT Information on sending your tick in for testing at TICK ;REPORT.
Test Your Tick at TICKNOLOGY Information on sending your tick for testing to TICKNOLOGY
Lyme Facts and Resources Lyme Disease: Need to Know Information.
Lyme Support Group Sign Up for Our Lyme Disease Support Group
Understanding Chronic Lyme Disease: A Whole System Approach
The Emergence of Lyme Disease
Lyme disease has been an elusive diagnosis. In 1975, in Lyme, Connecticut, there emerged clusters of children and adults with unusual symptoms of joint swelling and severe pain. The first 51 cases of Lyme were outlined two years later and a connection was made between the disease and the Ixodes Scapularis tick.
Finally, in 1982, Borrelia burgdorferi was unveiled as the bacterium that causes Lyme. The disease did not become reportable until 1987 when physicians were required to report all cases. 1
As stated in Holistic Primary Care, “Back in the 1990s, the prevailing conventional wisdom was that Lyme disease is a simple, relatively rare disorder that’s easy to avoid, difficult to acquire, simple to diagnose, and easily treatable with a single 30-day course of antibiotics” (p. 1). 2
Today, experienced doctors and frustrated patients tell a different story.
Chronic Lyme: Reality or Myth?
Over the last ten years, the incidence of Lyme disease has doubled. The current, heavily debated, enigmatic position by practitioners on Lyme questions whether or not it is a real medical condition caused by a bacterial infection or a psychological condition.
Based on our experience at the Stram Center and the available research, we believe that chronic Lyme disease is, in fact, a real condition as a result of the persistent presence of Lyme disease and/or its co-infections and/or the results of inflammatory proteins released by the bacteria.
Problem with a Simple Approach to the Complexity of Lyme
Fading importance of the Bulls-Eye
Currently, conventional medicine, when it does acknowledges the condition, centers around a tick bite, a bulls-eye rash, and a simple, short-term treatment of antibiotics. This simplistic approach is further aggravated by the complexity of acquiring a definitive laboratory diagnosis and the fact that, according to Duchess County, which is the highest reporting county for Lyme, only 18% of patients recall ever being bit by a tick.
As pointed out in Holistic Primary Care (Fall 2011), “If you rely exclusively on the Centers for Disease Control and Prevention (CDC) diagnostic criteria, you’ll miss about 90% of cases, as very few patients fit the strict “classic” profile defined by CDC” (p. 4).2 We cannot accept the status quo.
The Elusive Lyme Bacteria
The Lyme bacteria is very resistant and has the ability to change into different forms based on the stressors of the body’s internal environment in which it lives. Consequently, chronic Lyme disease can persist even after the administration of an antibiotic regimen. 3
There are a plethora of studies on the high incidence of relapse following short-term antibiotic therapies.4 The various forms of the bacteria may require different antibiotic treatments to affect eradication. The bacteria is also slow-growing and is able to hide in areas such as nerve tissue, connective tissue, and joint spaces, causing the multitude of symptoms and rendering effective blood laboratory analysis challenging at best. The chronic form of Lyme is more difficult to diagnose and to treat due to the various and multiple symptoms that it causes.
Prevalence is Likely Underestimated
According to new CDC statistics, there are approximately 400,000 Lyme disease cases per year, not including those cases that are unreported or misdiagnosed.
New York State has the highest number of people reporting Lyme infection. According to the Center for Disease Control, only 10-12% of actual numbers are reported and approximately 94% of all Lyme cases come from just twelve states. Moreover, it typically takes an average of nine visits to various doctors before the diagnosis of Lyme disease is made. The percentage of patients being diagnosed at their first doctor’s visit is less than 2%; 50% of patients are told it’s in their head, while 30% are diagnosed with depression. And 80% are simply told the diagnosis is an unknown mystery. Everyday patients are suffering from real symptoms, eluding diagnosis and going untreated.
Need for Public Awareness
Learning from Past Mysterious Diseases
There runs a strong parallel between the misunderstanding of Lyme today and the misunderstanding of AIDS and other conditions throughout the 20th century.
There is a striking similarity in the sentiments by the patients in their diagnosis and treatment for Lyme as was the case over 20 years ago for AIDS. As put forth by Steve Epstein, PhD, “these diseases have in common the demand on the part of the sufferers that their mysterious condition be acknowledged as legitimately medical. Sufferers find themselves in a state of an anxiety provoking experience in which they question their own sanity precisely because of the realness of their experience in the face of public medical doubt.”5 In the same way that clinical attention, public awareness, and funding were brought to the issue of AIDS and other once-mysterious conditions, similarly today this must be done for Lyme.
Need for Policy Change
Disparity of Funding
There is a wide disparity in funding for Lyme disease compared to other diseases such as West Nile Virus.
In 2004, California Lyme Disease Association reported the government spent 18 times more funding West Nile Virus than it did for Lyme Disease despite Lyme Disease being reported nearly 8 times more than West Nile.6 Today, those numbers have not improved: the NIH budget for 2012 requests $25 million dollars with 150,000 Americans reported, compared to $46 million for West Nile Virus with only 3,630 Americans reported and the CDC funding request for 2012 is $5 million for Lyme and $20 million for West Nile Virus. 7
Professional Liability
In Health Affairs, Laurie McClellan sheds light on a critical aspect of the problem.
She states, “during my research, I’d discovered that a state medical board once had suspended this doctor’s license for prescribing long-term antibiotics. I felt like an outlaw entering that office—and also like someone desperate for help.” 8 Given the liability associated with the treatment of Lyme disease, a policy change is necessary in order for us to be able to effectively carry out this model. It is more necessary than ever that there be a forum in which patients and providers can feel comfortable, safe, and have evidence-based treatment approaches towards the eradication of this disease. Practitioners should not fear the suspension of their licenses and patients should not feel desperate for help in the pursuit of treatment of Lyme disease. Furthermore, insurance coverage must play a significant role in making access to proper treatment possible.
Stram Center Experience, Testing and Treatment
TESTING:The Stram Center recognizes the limitations in the current indirect methodology used by blood testing for Lyme disease. Certainly, some tests are better than others; we can use a variety of laboratories chosen for their sensitivity and accuracy, such as IGENEX, MDL, GALAXY. Yet, until we have a direct method of testing, lab tests still have their limitations as a sole diagnostic tool. The clinical diagnosis by Lyme literate medical doctor, is in the end the right procedure, as testing can still miss about 50-60% of cases, with false negatives. The CDC also states that Lyme disease is a clinical diagnosis based on the unreliable current serology. Together, with our clinical experience from over 10,000 Lyme patients coming to us from all over the US and Europe, and the cross reference of several lab tests, we are confident in our diagnosis of Lyme disease and other tick borne illnesses.
TREATMENT: At the Stram Center, our practitioners are trained by the International Lyme and Associated Diseases Society, (ILADS) the foremost scientific and research organization for Lyme disease diagnosis and treatment. In addition, Dr. Stram has trained with Lyme experts in both the United States and Europe to develop his own unique protocols for treatment. Dr. Stram has been diagnosing and treating Lyme and co-infections since 2003 and has the clinical experience for working with more than 15,000 Lyme patients.
Given our clinical experience using the integrative model to treat our patients since 2003, we work first and foremost with the patient's story. This is also how we follow the progression of their disease and on to recovery.
We address the patient's lifestyle which includes diet, exercise, and social environments at work and home; we continue to monitor and review the biological terrain from which their medical condition is evaluated using state of the art laboratory analysis, including and not limited to Lyme testing, immunological testing, nutrient testing, and potentially stool and urine testing as well.
Our treatment is based on honoring the interconnection of the whole person, the pathology they are faced with and the multitude of treatment options that are available. We pool this knowledge together, with the patient, to formulate a customized treatment plan.
This plan will include:
- utilization of food as medicine;
- assessing nutritional intake;
- judicious and safe use of antibiotics when appropriate;
- nutritional and herbal supplements when appropriate;
- manual therapies such as acupuncture to augment treatment
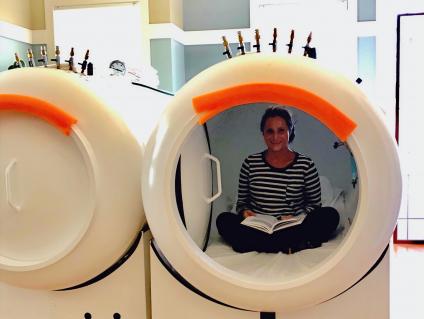
Hyperbaric Oxygen Therapy and Lyme Disease: Turning the corner on treatment progress
Hyperbaric oxygen therapy HBOT has been shown to elevate tissue oxygen, which can be lethal to Lyme bacteria, increase white blood cell activity and enhance antimicrobial responses. Oxygen is essential in the killing of bacteria and by exponentially raising oxygen levels through the body, the efficiency of bactericidal action of white blood cells can be enhanced dramatically.
Clinical data and case reports have demonstrated the lasting benefits of HBOT for Lyme disease with the following:
Ameliorate Neurological conditions:
- decreases neuroinflammation
- enhances short-term memory
- reduces chronic fatigue
- improves concentration
- ameliorates chronic headaches
- lessens depression
- moderates insomnia
Increase Mobility with HBOT:
- diminishes inflammatory-related arthritic pain
- lessens muscle discomfort
- improves walking distance
- amplifies energy levels
Enhance Antibacterial Effects with Hyperbaric Oxygen Therapy
- induces angiogenesis to mobilize blood flow to affected tissue and bone
- augments antibiotic interventions by driving spirochete out of biofilms
- enhances white blood cell and immune system activity
- improves antibiotic cell wall penetration
- increases oxygen free radicals to combat the Bb organism
The Stram Center practices medicine in a whole system approach to the care of our patients. Our treatment navigation is guided by listening to our patients tell their unique story.
Sarah's Story: Parents seek treatment for daughter at Delmar clinic after they say Irish doctors misdiagnosed her paralysis
DELMAR, N.Y. (NEWS10) — When doctors in Ireland claimed a little girl’s paralysis was psychosomatic, her parents refused to accept the diagnosis and instead travelled thousands of miles to a clinic in Delmar, New York where they say their 9-year old was successfully treated for Lyme Disease. Read Sarah's story
Joe's Testimonial: "The practice of Dr. Stram is the most incredible healing practice that I have ever been involved with."
Tia's Testimonial: " Dr. Stram and his team have been a Godsend." Read more from Tia
Make an Appointment Today
Please call the Stram Center:
Delmar, NY office:518 689-2244 or Burlington, VT office: 802 891-3459 if you would like to make an appointment to address Lyme.
References
1. A Brief History of Lyme Disease in Connecticut Department of Public Health, State of Connecticut, 02 June 2008.
2. Goldman, Erik. "Shape Shifters, Hidden Accomplices & Nature's Dirty Needles: Confronting the Challenges of Lyme Disease." Holistic Primary Care Fall 12.3 (2011): 1+4.
3. " Chronic Lyme Disease - Real Disease or Medical Myth?"
4. “Impure Science: AIDS activism and the politics of knowledge.” Steve Epstein
5. "Disparity in Funding: Lyme vs. West Nile." California Lyme Disease Association, 2004.
6. “ Government Research Funding." ME/CFS Worldwide Patient Alliance, 2009. Mar. 2012.
7. " Chronic Lyme Disease: It's Time To Solve The Medical Mystery Inside An Enigma." McClellan, Laurie, Health Affairs
Integrative Treatment Options

IV Therapy for Chronic Illness
Chronic illnesses are on the rise in the US. From chronic Lyme disease, cancers, chronic fatigue, pain and more – patients are attempting to live their best lives while fighting a battle within. A patient’s response to chronic illness is unique – based upon many factors ranging from emotional response to the disease, individual physical symptoms, immune response and the duration of the…IV Therapy for Chronic Illness

Hyperbaric Oxygen Therapy
Dedicated to treating the root cause of illness and using the most advanced integrative methods in a safe environment, the Stram Center for Integrative Medicine, under the medical supervision of Dr. Ron Stram, will utilize the benefits of hyperbaric oxygen therapy (HBOT) to complement and enhance the healing process in both chronic and acute conditions of our patients. You will…Hyperbaric Oxygen Therapy
Integrative Medicine
Integrative medicine is the blending of conventional medicine with holistic, complementary, and alternative medicine. Integrative Medicine is defined as healing-oriented medicine that takes account of the whole person (body, mind, heart and spirit), including all aspects of lifestyle. It emphasizes the therapeutic relationship and makes use of all appropriate therapies, both conventional and…Integrative Medicine

Chronic Illness
Nowhere is the need for an integrative approach more apparent than in the management of chronic illness. We are a synthesis of many systems all working together, and when one or more systems become diseased, all of the others will be stressed as well. From physical challenges, to the challenges of everyday living, to a satisfying quality of life, we have to go past seeing that illness in…Chronic Illness

Nutritional Counseling
The practitioners at the Center recognize that diet is often the basis for your heath and your potential to heal. Adopting a healthy diet is often the first step towards correcting health problems. Many medical conditions can be treated more effectively when the patient implements specific diets and uses nutritional supplements. These interventions afford fewer complications and side effects than…Nutritional Counseling
Tests We Use
The Stram Center for Integrative Medicine utilizes the most advanced and comprehensive testing available to assess root cause of illness for our established patients.A wide range of detailed and extensive diagnostic tests are accessible by the Stram Center and include highly sensitive and accurate testing . Aside from conventional medical testing, such as Complete Blood Counts,…Tests We Use

Supplements and Vitamins
Our natural remedies and supplements are carefully selected by our doctors and may be taken to promote natural healing and help treat a variety of conditions.Supplements and Vitamins