Medical Marijuana Comes to the Stram Center for Added Options for Patient Symptom Control

The Stram Center is pleased to be able to prescribe medical marijuana to patients meeting required NYS mandated criteria.We believe that medical marijuana will be a good symptom control option for patients not adequately benefiting from conventional pharmaceutical symptom control options for the qualifying conditions.
Medical marijuana, a controlled substance and classification in the United States as a Schedule I agent with high potential for abuse, is now able to be prescribed in designated forms by registered physicians for specified indications.It is derived from the Cannabis plant (including Cannabis sativa and Cannabis indica species), and this plant has been used in medicine for thousands of years prior to achieving its current status as an illicit substance.
The human body has an endocannabinoid system, comprised of receptors or binding sites for cannabinoid substances which are either made in the body or taken in from outside the body.CB1 receptors are found primarily in the brain, and CB2 receptors function in our immune system and are anti-inflammatory.
Two major components of cannabis include THC (Delta-9-tetrahydrocannabinol) and CBD (cannabidiol). THC is responsible for the therapeutic effects of cannabis use such as decreasing nausea and vomiting, increasing appetite, decreasing pain, and increasing muscle relaxation. It can however cause dizziness, sleepiness, and disorientation and has psychoactive properties. CBD alleviates anxiety, decreases seizures, relaxes blood vessels, causes pain relief, and is anti-inflammatory. The relative ratios of THC and CBD vary in the different allowable medical marijuana products available from NYS dispensaries.
In NYS, in order to receive a prescription for medical marijuana from a registered prescribing NYS physician, a patient must be diagnosed with one of the qualifying conditions listed: cancer, HIV/AIDS, amyotrophic lateral sclerosis (ALS), Parkinson’s disease, multiple sclerosis, spinal cord injury with spasticity, epilepsy, inflammatory bowel disease, Neuropathy or Huntington’s disease. In addition to the qualifying condition, one of the following associated conditions must be present: Cachexia (wasting syndrome), severe or chronic pain, severe nausea, seizures or severe or persistent muscle spasms.
The prescribing NYS physician will need to complete a special medical marijuana prescription through the Health Commerce website, specifying the mode of medical marijuana delivery (vaporized/inhaled, oral/mucosal, oral capsule) as well as ratio of THC :CBD (1:9, 1:1, or 9:1). The patient would need to acquire a registration card through NYS in order to receive the prescribed medical marijuana. The medical marijuana would be obtained from specific NYS dispensaries. The dispensaries give recommended dosing through their pharmacists, and doses are readjusted based on patient response.
Meditating for Peace Locally

Listen to guided Meditation online
If you are a regular at our weekly meditations, and are messing joining the group, you can listen to Meditation facilitator Jim Whiting lead meditation online. In January, Jim recorded a guided meditation and spoke about the Stram Center with the Albany Peace Project’s Bethany Gonyea.
The link is below;
Meditation and Yoga Cancelled While We Move

Yoga and Meditation are cancelled from February 1st thru the 22nd.
Beginning the first week of February Meditation and Yoga classes will be cancelled until we move in the new space. As we prepare to move into our new home the upstairs will be closed. We will resume in our new home the week of February 22nd. See you there! Any questions, please call the Center at 518-686-2244.
Meditation Can Improve Your Life

Meditation Can Improve Your Life.
Find out how Mediation can relieve stress and bring grace and ease into our life's journey. Join us tonight as we continue weekly guided meditation in our new space at 90 Adams Place.
7:30 PM. Free to all.
Meditation Promotes Health and Well-being for Physicians and for You
A study out of the University of Rochester shows that meditation and the opportunity to share emotions in a non judgmental way helps decrease physician stress while enhancing an experience of connectedness between physician and patient. The study, recently published in JAMA (9/23/09) was authored by a group led by Michael Krasner, M.D. They found that, with the meditation practices, physicians experienced a greater sense of well-being and satisfaction with their work.
Meditation, focused breathing, and the teachings which help one train the mind to be present with what is and those practices which help us deal skillfully with relationships and choices from a deep Inner Wisdom, are invaluable. Without any negative side effects, and in no way obstructing a person’s current medical regimen, these practices help one slowly “heal” those limitations which prevent us from attaining the health, happiness, and lives we desire.
Physicians as well as other healthcare practitioners often experience intense levels of stress which then lead to mental and emotional dis-ease, physical disease, difficulties in relationships, marital discord, feelings of resentment and inadequacy, and significant burnout and dissatisfaction with life. The stresses include time pressures, internal and external pressures to “be perfect” or to “never make a mistake”, and financial pressures due to overwhelming student loan payments. With training in practices such as meditation, physicians will not only feel better and be able to connect with their patients in a more heart-centered and connected way, but they will be able to then pass on these non-invasive yet powerfully health-supporting skills to their patients.
Meet our new Guided Meditation Teacher, Janaki Ramkumar

I was born and raised in India and left there after earing my Masters in Statistics. I came to the US 15 years ago. To stay connected to my orthodox Hindu family roots, I teach the Indian Heritage class at Albany Hindu Temple. The Heritage class helps children to understand their Indian Heritage. The curriculum is designed by Pujya Dyananda Saraswatiji of Arsha Vidya Gurukulam in Pennsylvania. Teaching this class gave me the opportunity to visit the Ashram and attend their meditation retreats. The first time I did meditation I wasn't sure whether I could do it! But, as I meditated more, it got better and better; that is the process by which I encourage others in their journey. I'm also a member of the Interfaith Story Circle of Albany. This gave me the opportunity to tell spiritual stories. I wanted to combine storytelling and meditation together. I started visiting the meditation sessions at the Stram Center a year ago and began telling spiritual storied at the end of the session to offer inspiration and help deepen the experience. I was also invited to do a meditation and storytelling session for Camp Braveheart. The experience has been overall so rewarding that I have made it part of my practice as a meditation teacher.
Melanoma: A Guide For Early Detection
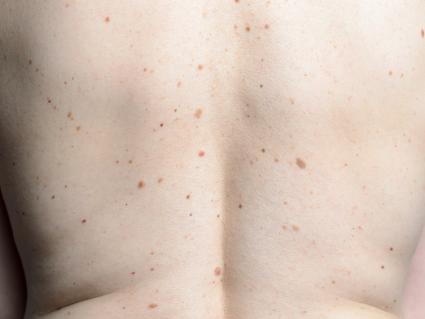
Prevention and early detection is key for melanoma.
Did you know that skin cancer is the most common of all types of cancer? This is, in fact, true.
Skin cancer can be divided into two major groups, melanoma and nonmelanoma (primarily squamous cell and basal cell) cancers. Malignant melanoma, the deadliest form of skin cancer, is a tumor that arises from cells called melanocytes which are found in the skin in what is known as the basal layer of the epidermis. Malignant melanoma is the fifth leading cause of cancer in men (5%) and the sixth leading cause of cancer in women (4%). Lifetime chance for development of invasive melanoma increases with age, and whites have a higher (10-fold) incidence than that of non-whites.
- Basal cell cancer is the most common type of skin cancer overall (75%) and arises from cells called basal cells which are found in the epidermis and also in hair follicles and sweat ducts
- Basal cell skin cancers can have the following presentation: flat, firm, pale or yellow areas similar to a scar; itchy, raised, reddish patches; small pink or red translucent or shiny, pearly bumps which could have blue, brown, or black areas; pink growths with raised edges and a lower area in their center which may contain abnormal blood vessels; or open sores with oozing and crusting that either don’t heal, or heal for a while but then come back
- Squamous cell cancer is the second most common type of skin cancer (20%) and arises from scaly cells found on the surface of skin
- Squamous cell skin cancers can appear as rough or scaly red patches which might crust or bleed; raised growths or lumps with a lower central area; open sores that ooze or crust and don’t heal, or heal but return again; or wart-like growths
What is a major cause of skin cancer?
- Ultraviolet (UV) light exposure and sunburns appear to be causative in all types of skin cancers, both melanoma and nonmelanoma skin cancers
- Ultraviolet A radiation can lead to development of melanoma and squamous cell skin cancer by producing reactive oxygen species
- Ultraviolet B radiation causes oxidative stress, DNA damage and impairment of repair, premature aging of the skin, and multiple effects on the immune system
- Other risk factors for malignant melanoma include:
- Personal or family history of melanoma
- Weakened immune system or immunosuppressive therapy, and higher socioeconomic group. Immunosuppression also increases risk for squamous cell skin cancer.
Measures to minimize UV light exposure of skin can be protective for all types of skin cancer.
How can you make a difference? Early detection of both melanoma and nonmelanoma skin cancers is important to assure early treatment and prevention of debility, and, in particular with melanoma, possible death.
- Self examination of your skin, with possible assistance of spouse or family members, should be done monthly, and can be an effective screening strategy to identify any new suspicious skin lesions, and this should be encouraged
- The American Cancer Society screening guidelines recommend regular skin self-examination for all adults. Pamphlets for self-examination of the skin are available from the American Cancer Society, the American Academy of Dermatology, and the Skin Cancer Foundation
- Clinical examination of the skin by a dermatologist should be done yearly for individuals at high risk for skin cancer (these could include those with a family or personal history of skin cancer and those with a high number of pigmented moles, or those with specific syndromes such as xeroderma pigmentosum or basal cell nevus syndrome)
Your self-skin exam is best done in a well-lit room in front of a full-length mirror. A hand-held mirror can be used to look at areas that are hard to see, such as the backs of the thighs. A family member can help by looking at the back and scalp. Getting familiar with location and size of existing moles is important. It is best to do these exams after a bath or shower, and, of course, to be thorough!
It is important that you recognize the difference between normal and suspicious moles.
- A normal mole is usually an evenly colored brown, tan, or black spot on the skin. It can be either flat or raised, and either round or oval. Moles are usually less than 6 millimeters (1/4 inch) in size, about the width of a pencil eraser. Moles can be present at birth, or arise during childhood or young adulthood; new moles that appear later in life should be checked by a health care provider
- The most important warning sign for melanoma is a new mole on the skin or a mole that is changing in size, shape, or color
- Another important sign is a mole that looks different from all the other moles on the skin. These too should be checked by a health care provider
The “ABCDE” screening guideline is helpful to guide detection of melanoma (you can see color images of normal and abnormal moles at www.skincancer.org; I highly recommend you take a look!) The guideline is as follows:
- Asymmetry: one half of the mole does not match the other
- Border: mole edges are irregular, ragged, notched, or blurred
- Color: color is patchy and not the same all over, may include shades of brown, black, pink, white, blue
- Diameter: mole is larger than 6 mm across (although sometimes melanomas are smaller than this)
- Evolving: mole is changing in size, shape, or color over time
However, some melanomas do not “fit” the ABCDE guidelines and may present as: a sore that does not heal; spread of pigment from the border of a mole into the surrounding skin; redness or a new swelling beyond the border of a mole; itchiness or pain in a mole; or change in the surface of a mole (scaliness, bleeding or oozing of a mole).
Fortunately, imaging studies such as xrays and CT scans are not needed for early detection of skin cancer--just careful visual exam of the skin. So grab a mirror and start inspecting!
Men’s Health at a Glance

Men interested in impacting their prostate cancer risk can be pro-active in their lives, and integrate these measures along with their screening routines to give themselves the best chance for good health!
A significant number of men are concerned about their risk for developing prostate cancer. This is especially relevant now since the frequency of monitoring PSA values has been in recent debate amongst groups who develop screening guidelines. Although all men are at risk for prostate cancer, there are known factors that increase a man’s chance of its development, such as: increasing age, family history of blood relatives having prostate cancer, African American race, obesity, tobacco use/smoking cigarettes, consumption of high fat diet (saturated and trans-fats), occupational exposure to pesticides and chemicals (ex: farming, lawn care, exterminator), and having an initial PSA level of > 2 ng/mL; abnormal percentage of free PSA; elevated PSA velocity.
So other than screening for prostate cancer (in other words, secondary prostate cancer prevention), which usually includes yearly digital rectal exam, PSA blood test (frequency of which is controversial), and documenting any changes in urinary symptoms, how can men be proactive in decreasing their risk (primary prevention)? We know that there are certain lifestyle habits and supplements that can have an impact in decreasing men’s risk for prostate cancer. These include the following:
- Exercise: Physical activity and aerobic exercise can reduce prostate cancer risk by lowering body fat and serum testosterone concentration. Exercise also can lessen the risk for developing more aggressive or advanced prostate cancer. Men should exercise 30 minutes or longer at least three times weekly.
- Pesticides/Endocrine Disruptors: A xenobiotic or endocrine disruptor is any chemical or toxin that is foreign to the body and can mimic natural hormones. An example is Agent Orange (dioxin) exposure in veterans, which has doubled the risk for prostate cancer and is particularly linked with more aggressive prostate cancers at younger ages. Chemicals in plastic, ink, electronic equipment, and personal care products such as skin moisturizers and deodorants also can increase one’s risk. Farm raised meat additionally is a source of toxic pesticides and hormones. Taking supplements that contain androgens (male hormones), and a supplement for bone health (chondroitin sulfate) in men at higher risk is not advised. Actively avoiding chemicals that are endocrine disruptors can decrease risk.
- Alcohol: Excessive drinking of alcohol can increase prostate cancer risk (for example, in one study, 10 drinks of alcohol per week tripled the risk). Avoiding excessive amounts of alcohol can decrease risk.
- Smoking: Tobacco contains cadmium, a heavy metal that may increase prostate cancer risk, so avoiding cigarette smoking and tobacco use is prudent for risk reduction.
- Nutrition: Excessive calories and consumption of animal/saturated fat (especially from dairy and red meat, rich in omega-6 fatty acids) increase prostate cancer risk, so limiting these can impact risk. Eating fewer calories and more omega-3 rich foods such as fish and olive oil are protective. Soy consumption, particularly non fermented soy such as in soy milk, soy cheese, edamame and tofu, is protective for prostate cancer. Daily consumption of at least 4 ounces of soy protein is helpful for prostate cancer prevention. Lycopene, found in tomatoes, strawberries, watermelon, and apricots, is also protective for prostate cancer, and cooking the tomatoes and adding some olive oil is especially helpful to allow release and absorption of lycopene. Eating a plant-based diet, rich in the cruciferous vegetables (broccoli, Brussels sprouts, kale, etc.) also decrease prostate cancer risk. Pomegranate juice, which contains ellagic acid, can inhibit prostate cancer cell growth, so men should consider consuming 8 ounces of pomegranate juice daily. Finally, green tea contains antioxidants called catechins that have antitumor activity against prostate cancer cells, and drinking 3-5 cups of organic decaffeinated green tea per day is recommended for prevention.
- Supplements/Medications: Vitamin D deficiency has been associated with an increased risk for development of prostate cancer, so getting adequate production of vitamin D by sun exposure and by supplementation if needed is recommended for prevention. Maintaining a vitamin D level of at least 30 mn/mL for prevention of prostate cancer and a level between 50 and 100 ng/mL for men with prostate cancer is recommended. Aspirin, by its reduction of inflammation, has been shown to decrease the risk for prostate cancer when taken for 5 years or more. If there are no medical contraindications to taking aspirin, men should take a baby dose aspirin of 81 mg daily for prostate cancer risk reduction.
- Mind-Body Medicine: Because stress can reduce the strength of one’s immune system, in particular suppressing natural killer (NK) cell activity (cells which typically fend off cancer cells), incorporating mind-body therapies into one’s lifestyle can be helpful for prostate cancer prevention. Numerous such therapies are available, including meditation, yoga, and Reiki, and others, and men may wish to practice those they feel comfortable with.
Men interested in impacting their prostate cancer risk can be pro-active in their lives, and integrate these measures along with their screening routines to give themselves the best chance for good health!
Move More, Age Less

Our bodies need movement to function optimally. Movement stimulates the lymphatic system, helps blood circulation, increases energy, decreases anxiety, improves sleep, and keeps muscles and joints working properly. Technological advances have made our lives easier, but the downside is a tendency to adopt a sedentary lifestyle. Sitting at a computer all day, binge watching television (we don’t even have to get up to turn the channel) and driving instead of walking are just a few examples...
Our bodies can handle a lot, but over time inactivity, poor posture, and repetitive motions like looking down at your phone while texting, can create asymmetries in the body. These asymmetries cause aging symptoms to appear like chronic pain and stiffness.
In my myofascial massage practice, two common problems I see are rounded shoulders with head forward posture, which can lead to back, shoulder and neck pain, and tight hip flexor muscles (psoas muscles) from sitting too much, which can cause low back pain. Massage is a great way to correct asymmetries. In addition, I also recommend movement at home for my clients as the most important work is how you take care of yourself on daily basis.
It is never too late to add activity to your life. Adding just a few minutes of stretching and walking can make a big difference in how you feel now and, in the years, to come. As always, it is a good idea to check with your physician before beginning a new exercise regimen to be sure your body does not need special precautions.
Keep your body moving and enjoy the benefits of your healthy lifestyle!
Multi-Vitamins ? Are They Safe?
While a recent NBC News article and recent studies have been promoting the concept that multi-vitamins (MVI) are not safe or appropriate to take, MVI do show promise in being a useful part of an optimal health plan.
The recent studies that are circulating around in the media are dismissing MVI due to their lacking evidence that their usage did not prevent cancer, heart disease, and other causes of death. There are several problems with these claims. There are many factors that go into risk for diseases such as cancer and heart disease. While these studies do their best to control for other factors that could influence the results, it is impossible to control all of the risk factors for cancer and heart disease. Lifestyle plays a huge role in prevention and management of disease. Lifestyle can be defined as ones diet, exercise, sleep, and stress management practices.
Taken For Wrong Reasons?
Many times MVI are taken for the wrong reason. They are not meant to prevent disease, combat fatigue, increase mental acuity, etc. The main reason for a MVI is to help support a healthy diet in supplying an individual with the nutrients they need to survive and hopefully thrive.
While it is important that these studies assess the impact of interventions on large groups of people, supplementation should be individualized and managed by a qualified health practitioner, such as a Medical Doctor, Naturopathic Doctor, Physician’s Assistant, Nurse Practitioner, or a Registered Dietitian. There may be other specific nutrients that would be more appropriate for an individual than a MVI alone, but one may have difficulty determining this on their own.
There also is research showing negative effects of MVI on specific populations or related to the combination of MVI with other supplements. This typically happens when people take a MVI or other supplements that are inappropriate for their needs. At The Stram Center for Integrative Medicine, a patient’s nutrition plan is individualized so that each person has their specific needs met.